Here’s one of the most challenging and thought-provoking articles I’ve read for a long time. It’s by Sharon Begley and the title is “The Depressing News about Antidepressants”. A lot of people take antidepressants and the consumption is increasing. In the US it’s doubled in a decade (from 13.3 million in 1996 to 27 million in 2005). Most of these people say the antidepressants help them (about 3 out of every 4 people say that).
However, researchers such as Irving Kirsch, of Hull University, have been looking closely at the evidence base to see how much of the benefit can be attributed to the drugs, and how much to the placebo effect.
In 1998 they reviewed 38 trials (all of which were sponsored by the manufacturers of the drugs) and found that in the 3000 patients studied, those who received placebo demonstrated about 75% of the improvement experienced by those on the drugs. Now you might think that means the drugs were more effective than the placebo, and that’s true, but how much more effective? One of the mistakes people often make when reading clinical trials is to assume that in the two groups, the placebo group and those taking the drug, that the placebo effect only occurs in the placebo group. That’s not true, however. The placebo effect occurs in everyone and the results of those trials suggest that three quarters of the improvement experienced by those taking the antidepressants is due to the placebo effect, and only a quarter to the actual drug.
Kirsch then went on to examine unpublished trials. He found that 40% of the trials of these drugs were unpublished (across the board an average of 22% of clinical trials are unpublished so this was an unusually high proportion). He found that in over half of the unpublished studies the drugs performed no better at all than placebo. This pushed the placebo effect in antidepressants up from 75% of the overall effect to 82%. The additional 18% difference was hardly clinically significant (amounting to only 1.8 point extra improvement in the 54 point depression rating scale)
In January this year, Hollon, DeRubeis and others published, in JAMA, their own review of clinical trials of antidepressants and concluded
“Most people don’t need an active drug,” says Vanderbilt’s Hollon, a coauthor of the study. “For a lot of folks, you’re going to do as well on a sugar pill or on conversations with your physicians as you will on medication. It doesn’t matter what you do; it’s just the fact that you’re doing something.” But people with very severe depression are different, he believes. “My personal view is the placebo effect gets you pretty far, but for those with very severe, more chronic conditions, it’s harder to knock down and placebos are less adequate,” “Prescribers, policy-makers, and consumers may not be aware that the efficacy of [antidepressants] largely has been established on the basis of studies that have included only those individuals with more severe forms of depression,” People with anything less than very severe depression “derive little specific pharmacological benefit from taking medications. Pending findings contrary to those reported here … efforts should be made to clarify to clinicians and prospective patients that … there is little evidence to suggest that [antidepressants] produce specific pharmacological benefit for the majority of patients.”
The Newsweek article goes on to consider the issues of using increasingly high doses of antidepressants and switching from drug to another, but nothing shakes the conclusion that by far and away the greatest effect of antidepressants is from the placebo effect. The author also considers the serotonin story showing that lowering brain levels of serotonin appears to have no effect on mood which makes it hard to swallow the theory that SSRIs (Serotonin Selective Reuptake Inhibitors), the most modern form of antidepressant, like Prozac, relieve depression by altering serotonin levels.
But wait! As Jonah Lehrer points out in his excellent post on this article, there is evidence that SSRIs might increase brain plasticity – in other words, maybe they make it easier for you to cope, so let’s not throw them away yet!
So, here’s the first disturbing part of this article – antidepressants are, for most people, not any more beneficial than placebos.
What’s the second issue?
What do we do about that?
A major theme of the article is the “moral dilemma” involved in sharing this knowledge. The point that Sharon Begley makes in this article is that we know the placebo effect is highly dependent on the patient’s expectations and beliefs about the treatment they are receiving (in other words, if you tell someone their treatment is “only” as good as placebo), then the benefit they were experiencing disappears (or at least reduces substantially). Here’s the summary of the argument –
Friends and colleagues who believe Kirsch is right ask why he doesn’t just shut up, since publicizing the finding that the effectiveness of antidepressants is almost entirely due to people’s hopes and expectations will undermine that effectiveness. Kirsch, he insists that it is important to know that much of the benefit of antidepressants is a placebo effect. If placebos can make people better, then depression can be treated without drugs that come with serious side effects, not to mention costs. Wider recognition that antidepressants are a pharmaceutical version of the emperor’s new clothes, he says, might spur patients to try other treatments. “Isn’t it more important to know the truth?” he asks. Based on the impact of his work so far, it’s hard to avoid answering, “Not to many people.”
This dilemma is such a dilemma in part because the placebo response is so poorly understood, and, I believe mis-conceptualised (cripes! is there such a word?) In particular, many people make the erroneous assumption that a placebo is no better than doing nothing, and/or that it’s effects are only temporary, so not ultimately useful. Neither of these assumptions is justifiable. A benefit, or a harm, from a placebo, or nocebo, can be both powerful and long-lasting.
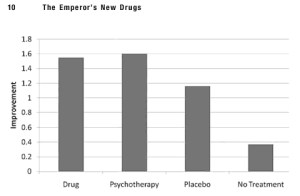
Kirsch has a new book out entitled “The Emperor’s New Drugs”. In the opening pages he includes this excellent graph.
What the graph shows so clearly is not only that the drug effect is not that much greater than the placebo effect, but that the placebo effect is considerably greater than doing nothing. I think this is a key point which is commonly missed, and which we need to address. If you think the placebo effect is no better than doing nothing, you’ll argue that any treatment which is not significantly greater in its effect than the placebo effect should be withdrawn. But then what? What if everyone who is currently taking antidepressants stopped them because they are no better than placebo? The amount of mental distress and harm would probably go through the roof. Kirsch is at pains to specifically warn against this response in the front of his book.
This is a complicated question. It’s not as simple as dividing treatments into those “which work” and those “which don’t work” on the basis of placebo controlled trials.
Don’t we need to approach this problem from a different angle? Human beings are complex adaptive organisms. Complex adaptive organisms self-organise. That’s a fundamental characteristic of all complex adaptive systems. Self-organisation in human beings includes defence and repair. There is no way for anyone to heal other than through the effective functioning of our self-organisation, or to put it another way, we only become well through the effects of self-healing. It doesn’t matter whether someone receives a drug or a placebo, if they are genuinely healing, it’s self-healing that’s doing it – in both cases. Drugs, at best, are adjuvants to that process. They support the organism as it self-heals.
The question then is what treatments support and promote self-healing? The second question is what potential harms can those treatments cause? A choice about treatment then involves balancing these two aspects – the potential for healing vs the potential for harm. As well as comparing treatment options this way, we then need to set this against what we’d expect might happen if we did nothing.
I don’t think any of this is easy, and I certainly don’t think I’ve got it all worked out myself yet either, but isn’t it time we started to think about health care differently?
As I said at the start of this post, this is one of the most disturbing and thought-provoking articles I’ve read for a long time. (I’ve added The Emperor’s New Drugs to my reading list!)

Great article. In many cases antidepressants are being prescribed by the family doc instead of psychiatrists which appears to reduce the cost of medical care (fewer specialists involved) but creates a class of patients on high powered drugs with little oversight. So if we take away the placebo effect we may effectively take away the only source of treatment for many people.
[…] graph is from Irvin Kirsch’s “Emperor’s New Drugs“. It clearly shows that placebo and doing nothing are not the […]
[…] is not the same as doing nothing. Kirsch makes that very clear in the introduction to his book, “The Emperors New Drugs” where he shows the difference in depression between placebo groups and no treatment groups. But […]
[…] I should send Dr Gerada a copy of Irving Kirsch’s excellent summary of the evidence base for antidepressants. I think he makes it very clear that the issue of antidepressant prescribing is […]
Are you sure that brain plasticity equates to coping? That assumes that any changes are for the better. But another of Kirsch’s assertions is that the drugs alter the physical brain so that the drug-takers experience perma-depression for the duration of their lives.
Em, no. I don’t think that’s what I said, but if it is, it’s not what I meant to say.
I think brain plasticity is one of the potentially adaptive mechanisms that we humans possess. Whether the changes which emerge in the brain are “good” or “bad” is only revealed in the living it. Not all changes in our brains or our bodies can be described as “healing”. Some clearly are damaging, pathological even. However without the ability to change we are stuck. What plasticity is good for is flexibility, or the potential to change and/or adapt.